Department of Pathophysiology and Host Defense
The Department of Pathophysiology and Host Defense comprises divisions of Pathophysiology, Immunology, Animal Experiment and Senior Researcher section. In the Divisions of Pathophysiology and Immunology, we aim to analyse infection, development, and recurrence of tuberculosis and other mycobacterial diseases at molecular levels. We also try to elucidate their pathophysiological mechanisms.
The Division of Animal Experiment supports basic research using experimental animals. The Senior Researcher section is responsible for projects on novel anti-mycobacterial drugs and combinational chemotherapy and implementation of pharmacological studies.
Collaborative research projects with developing countries
We have been conducting collaborative researches with Vietnamese institutes through NCGM-BMH Medical Collaboration Center for more than 10 years. Our research projects include host immunogenetics; host-pathogen interactions; and clinical epidemiology on mycobacterial infection, development, and recurrence of the disease. Particularly, control of multi-drug resistant tuberculosis is an important target.

Research on human susceptibility genes and molecular pathogenesis of airway infectious/inflammatory diseases
We have been investigating the functional significance of airway defense genes and their polymorphisms. We have so far identified novel mucin genes on the human sixth chromosome and characterization of these genes is underway. Our target genes include beta-defensins and interferon-inducible anti-viral genes as well. This would help us to understand pathogenesis of airway infectious/inflammatory diseases widely.
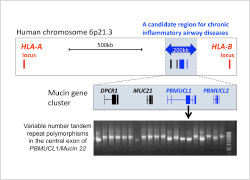
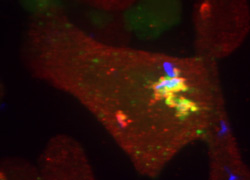
Unique strategy of intracellular parasitism of Mycobacterium tuberculosis
M. tuberculosis is an intracellular bacterium, which can proliferate within phagocytosed macrophages. M. tuberculosis gains this ability by escaping from the killing and digesting mechanisms of macrophages. We have been studying the unique strategy of its intracellular parasitism by investigating the membrane trafficking in infected macrophages.
Research on TB pathogenesis using animal models
M. tuberculosis can infect not only humans but also animals such as mice. However, susceptibility to M. tuberculosis infection varies among animals, and the histopathology of mice differs from that of TB. Recently, a TB mouse model has been developed that is thought to reflect human active TB. Using this mouse model, we are studying the host and bacterial factors involved in TB pathophysiology.

Publication list in the past five years
-
Noguchi S, Hamano E, Matsushita I, Hijikata M, Ito H, Nagase T, Keicho N. Differential effects of a common splice site polymorphism on the generation of OAS1 variants in human bronchial epithelial cells. Hum Immunol 74 (3): 395-401, 2013.
- hi S, Hijikata M, Hamano E, Matsushita I, Ito H, Ohashi J, Nagase T, Keicho N. MxA transcripts with distinct first exons and modulation of gene expression levels by single-nucleotide polymorphisms in human bronchial epithelial cells. Immunogenetics 65 (2): 107-14, 2013.
-
Pitabut N, Sakurada S, Tanaka T, Ridruechai C, Tanuma J, Aoki T, Kantipong P, Piyaworawong S, Kobayashi N, Dhepakson P, Yanai H, Yamada N, Oka S, Okada M, Khusmith S, Keicho N. Potential function of granulysin, other related effector molecules and lymphocyte subsets in patients with TB and HIV/TB coinfection. Int J Med Sci 10 (8): 1003-1014, 2013.
-
Hang NT, Maeda S, Lien LT, Thuong PH, Hung NV, Thuy TB, Nanri A, Mizoue T, Hoang NP, Cuong VC, Ngoc KT, Sakurada S, Endo H, Keicho N. Primary drug-resistant tuberculosis in Hanoi, Viet Nam: present status and risk factors. PLoS One 8 (8): e71867, 2013.
-
Hung NV, Ando H, Thuy TT, Kuwahara T, Hang NT, Sakurada S, Thuong PH, Lien LT, Keicho N. Clonal expansion of Mycobacterium tuberculosis isolates and coexisting drug resistance in patients newly diagnosed with pulmonary tuberculosis in Hanoi, Vietnam. BMC Res Notes 6:444, 2013.
-
Hang NT, Matsushita I, Shimbo T, Hong LT, Tam DB, Lien LT, Thuong PH, Cuong VC, Hijikata M, Kobayashi N, Sakurada S, Higuchi K, Harada N, Endo H, Keicho N. Association between tuberculosis recurrence and interferon-γ response during treatment. J Infect 69 (6): 616-626, 2014.
-
Hijikata M, Matsushita I, Hang NT, Maeda S, Thuong PH, Tam DB, Shimbo T, Sakurada S, Cuong VC, Lien LT, Keicho N. Age-dependent association of mannose-binding lectin polymorphisms with the development of pulmonary tuberculosis in Viet Nam. Hum Immunol 75 (8): 840-846, 2014.
-
Maeda S, Hang NT, Lien LT, Thuong PH, Hung NV, Hoang NP, Cuong VC, Hijikata M, Sakurada S, Keicho N. Mycobacterium tuberculosis strains spreading in Hanoi, Vietnam: Beijing sublineages, genotypes, drug susceptibility patterns, and host factors. Tuberculosis 94 (6): 649-656, 2014.
-
Hang NT, Maeda S, Keicho N, Thuong PH, Endo H. Sublineages of Mycobacterium tuberculosis Beijing genotype strains and unfavorable outcomes of anti-tuberculosis treatment. Tuberculosis 95 (3): 336-342, 2015.
-
Jeong S, Patel N, Edlund CK, Hartiala J, Hazelett DJ, Itakura T, Wu PC, Avery RL, Davis JL, Flynn HW, Lalwani G, Puliafito CA, Wafapoor H, Hijikata M, Keicho N, Gao X, Argüeso P, Allayee H, Coetzee GA, Pletcher MT, Conti DV, Schwartz SG, Eaton AM, Fini ME. Identification of a Novel Mucin Gene HCG22 Associated With Steroid-Induced Ocular Hypertension. Invest Ophthalmol Vis Sci 56 (4): 2737-2748, 2015.
-
Matsushita I, Hang NT, Hong LT, Tam DB, Lien LT, Thuong PH, Cuong VC, Hijikata M, Kobayashi N, Sakurada S, Higuchi K, Harada N, Keicho N. Dynamics of immune parameters during the treatment of active tuberculosis showing negative interferon-gamma response at the time of diagnosis. Int J Infect Dis 40:39-44, 2015.
-
Yatagai Y, Hirota T, Sakamoto T, Yamada H, Masuko H, Kaneko Y, Iijima H, Naito T, Noguchi E, Tamari M, Kubo M, Takahashi A, Konno S, Makita H, Nishimura M, Hijikata M, Keicho N, Homma S, Taguchi Y, Azuma A, Kudoh S, Hizawa N. Variants nearby the HLA complex group 22 gene confer increased susceptibility to late-onset asthma in Japanese populations. J Allergy Clin Immunol 138 (1): 281-283.e13, 2016.
-
Nakauchi A, Wong JH, Mahasirimongkol S, Yanai H, Yuliwulandari R, Mabuchi A, Liu X, Mushiroda T, Wattanapokayakit S, Miyagawa T, Keicho N, Tokunaga K. Identification of ITPA as a susceptibility gene to young-onset Tuberculosis on Chromosome 20. Human Genome Variation 3:15067, 2016.
-
Hijikata M, Matsushita I, Hang NT, Thuong PH, Tam DB, Maeda S, Sakurada S, Cuong VC, Lien LT, Keicho N. Influence of the polymorphism of the DUSP14 gene on the expression of immune-related genes and development of pulmonary tuberculosis. Genes and Immunity 17 (4): 207-212, 2016.
-
Thuong PH, Tam DB, Sakurada S, Hang NT, Hijikata M, Hong LT, Ngoc PT, Anh PT, Cuong VC, Matsushita I, Lien LT and Keicho N. Circulating granulysin levels in healthcare workers and latent tuberculosis infection estimated using interferon-gamma release assays. BMC Infectious Diseases 16 (1): 580, 2016.
-
Wada T, Hijikata M, Maeda S, Hang NT, Thuong PH, Hoang NP, Hung NV, Keicho N. Complete genome sequences of three representative Mycobacterium tuberculosis Beijing family strains belonging to distinct genotype clusters in Hanoi, Vietnam, during 2007–2009. Genome Announc 5 (27):2017. pii: e00510-17.
-
Wada T, Hijikata M, Maeda S, Hang NT, Thuong PH, Hoang NP, Hung NV, Keicho N. Complete genome sequence of a Mycobacterium tuberculosis strain belonging to the EAI family in the Indo-Oceanic lineage, isolated in Hanoi, Vietnam. Genome Announc 5 (24):2017. pii: e00509-17.
- Hijikata M, Keicho N, Duc LV, Maeda S, Hang NTL, Matsushita I, Kato S. Spoligotyping and whole-genome sequencing analysis of lineage 1 strains of Mycobacterium tuberculosis in Da Nang, Vietnam. PLoS One 12 (10): e0186800, 2017.
- p>Morimoto K, Hijikata M, Zariwala MA, Nykamp K, Inaba A, Guo TC, Yamada H, Truty R, Sasaki Y, Ohta K, Kudoh S, Leigh MW, Knowles MR, Keicho N. Recurring large deletion in DRC1 (CCDC164) identified as causing primary ciliary dyskinesia in two Asian patients. Mol Genet Genomic Med. 00:e838, 2019.
-
Maeda S, Hijikata M, Hang NTL, Thuong PH, Huan HV, Hoang NP, Hung NV, Cuong VC, Miyabayashi A, Seto S, Keicho N. Genotyping of Mycobacterium tuberculosis spreading in Hanoi, Vietnam using conventional and whole genome sequencing methods. Infect Genet Evol. 78:104107, 2020.
-
Keicho N, Hijikata M, Morimoto K, Homma S, Taguchi Y, Azuma A, Kudoh S. Primary ciliary dyskinesia caused by a large homozygous deletion including exons 1-4 of DRC1 in Japanese patients with recurrent sinopulmonary infection. Mol Genet Genomic Med. 00:e1033, 2019.
-
Hang NTL, Hijikata M, Maeda S, Thuong PH, Ohashi J, Van Huan H, Hoang NP, Miyabayashi A, Cuong VC, Seto S, Van Hung N, Keicho N. Whole genome sequencing, analyses of drug resistance-conferring mutations, and correlation with transmission of Mycobacterium tuberculosis carrying katG-S315T in Hanoi, Vietnam. Sci Rep 9(1):15354, 2019.
-
Seto S, Morimoto K, Yoshida T, Hiramatsu M, Hijikata M, Nagata T, Kikuchi F, Shiraishi Y, Kurashima A, Keicho N. Proteomic profiling reveals the architecture of granulomatous lesions caused by tuberculosis and Mycobacterium avium complex lung disease. Front Microbiol 10: 3081, 2020.
-
Hang NTL, Hijikata M, Maeda S, Miyabayashi A, Wakabayashi K, Seto S, Diem NTK, Yen NTT, Duc LV, Thuong PH, Huan HV, Hoang NP, Mitarai S, Keicho N, Kato S. Phenotypic and genotypic features of the Mycobacterium tuberculosis lineage 1 subgroup in central Vietnam. Sci Rep 11(1):13609, 2021.
-
Furuuchi K, Seto S, Nakamura H, Hikichi H, Miyabayashi A, Wakabayashi K, Mizuno K, Oka T, Morimoto K, Hijikata M, Keicho N. Novel Screening System of Virulent Strains for the Establishment of a Mycobacterium avium Complex Lung Disease Mouse Model Using Whole-Genome Sequencing. Microbiol Spectr. e0045122, 2022.
-
Seto S, Nakamura H, Guo TC, Hikichi H, Wakabayashi K, Miyabayashi A, Nagata T, Hijikata M, Keicho N. Spatial multiomic profiling reveals the novel polarization of foamy macrophages within necrotic granulomatous lesions developed in lungs of C3HeB/FeJ mice infected with Mycobacterium tuberculosis. Front Cell Infect Microbiol 12:968543, 2022.
-
Hikichi H, Seto S, Wakabayashi K, Hijikata M, Keicho N. Transcription factor MAFB controls type I and II interferon response-mediated host immunity in Mycobacterium tuberculosis-infected macrophages. Front Microbiol 13:962306, 2022.
-
Hijikata M, Morimoto K, Takekoshi D, Shimoda M, Wakabayashi K, Miyabayashi A, Guo TC, Yamada H, Keicho N. Analysis of Aberrant Splicing Events and Gene Expression Outliers in Primary Ciliary Dyskinesia. Am J Respir Cell Mol Biol 68(6):702-705, 2023.
-
Keicho N, Morimoto K, Hijikata M. The challenge of diagnosing primary ciliary dyskinesia: a commentary on various causative genes and their pathogenic variants. J Hum Genet 68:571-575, 2023.
-
Hang NTL, Hijikata M, Maeda S, Thuong PH, Huan HV, Hoang NP, Tam DB, Anh PT, Huyen NT, Cuong VC, Kobayashi N, Wakabayashi K, Miyabayashi A, Seto S, Keicho N. Host-pathogen relationship in retreated tuberculosis with major rifampicin resistance-conferring mutations. Front Microbiol 14:1187390, 2023.
-
Ito M, Morimoto K, Ohfuji T, Miyabayashi A, Wakabayashi K, Yamada H, Hijikata M, Keicho N. FOXJ1 Variants Causing Primary Ciliary Dyskinesia with Hydrocephalus: A Case Report from Japan. Intern Med. 2023 Oct 6. doi:10.2169/internalmedicine.2565-23.
-
Keicho N, Hijikata M, Miyabayashi A, Wakabayashi K, Yamada H, Ito M, Morimoto K. Impact of primary ciliary dyskinesia: Beyond sinobronchial syndrome in Japan. Respir Investig. 2024 Jan;62(1):179-186.
-
Horita Y, Doi N. Comparative study of the effects of antituberculosis drugs and antiretroviral drugs on cytochrome P450 3A4 and P-glycoprotein.Antimicrob Agents Chemother 58 (6): 3168-3176, 2014.
-
Horita Y, Maeda S, Kazumi Y, Doi N. In vitro susceptibility of Mycobacterium tuberculosis isolates to an oral carbapenem alone or in combination with -lactamase inhibitors.Antimicrob Agents Chemother 58 (11): 7010-7014, 2014.
-
Disratthakit A, Prammananan T, Tribuddharat C, Thaipisuttikul I, Doi N, Leechawengwongs M, Chaiprasert A. Role of gyrB Mutation in Pre-extensively and Extensively Drug-Resistant Tuberculosis in Thai Clinical Isolates. Antimicrob Agents Chemother 60 (9): 5188-5197, 2016.
-
Horita Y, Alsultan A, Kwara A, Antwi S, Enimil A, Ortsin A, Dompreh A, Yang H, Wiesner L, Peloquin CA. Evaluation of the adequacy of WHO revised dosages of the first-line antituberculosis drugs in children with tuberculosis using population pharmacokinetic modeling and simulations. Antimicrob Agents Chemother. 62(9), 2018. pii: e00008-18.
